Opioid addiction

Written by:

Medically Reviewed by:
Last Updated:
March 28th, 2025
Opiates are a medication prescribed to treat pain. While these are prescribed by doctors, they do, however, carry great potential for creating opiate addiction – particularly when people use them for longer than advised. In 2020, there were 2,263 opiate-related deaths in England and Wales.
One of the most interesting effects of opiates is how rapidly dependency develops for some users. Here, we’ll look at what the signs of addiction are, helping you to safely monitor the way you take your medication. If you think you might have developed an opiate addiction, you’ll also find what recovery support is available and advice on what to do next.
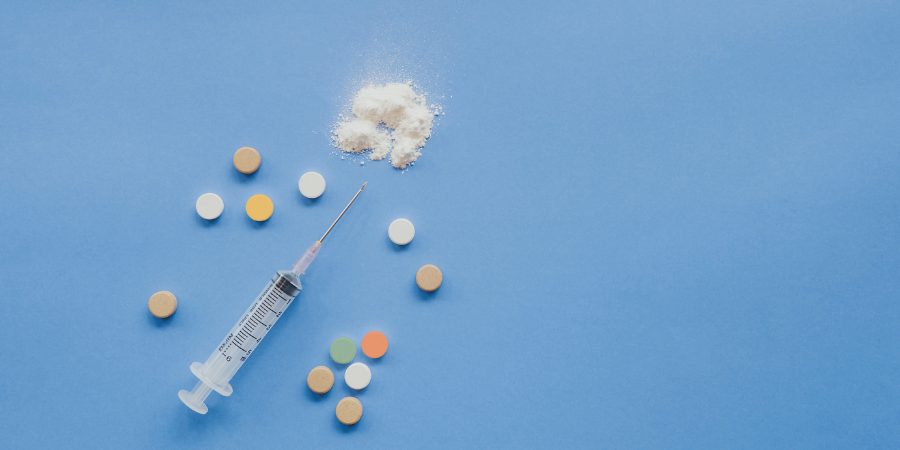
What are opiates and opioids?
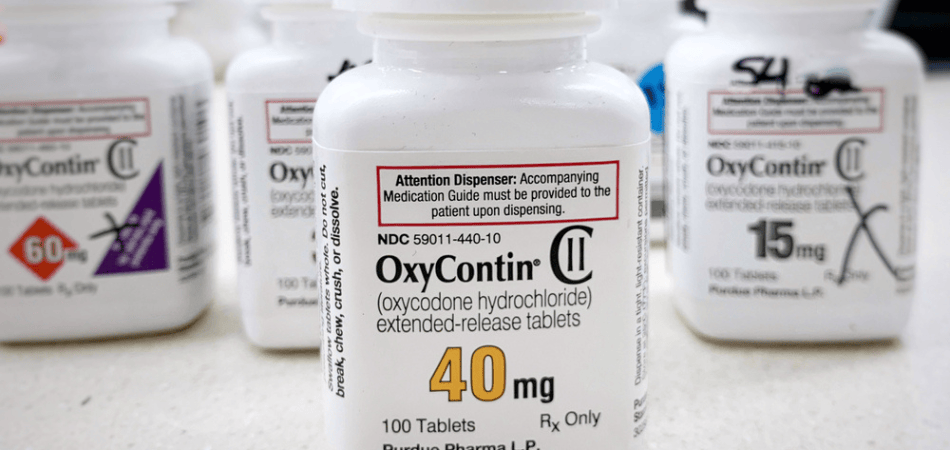
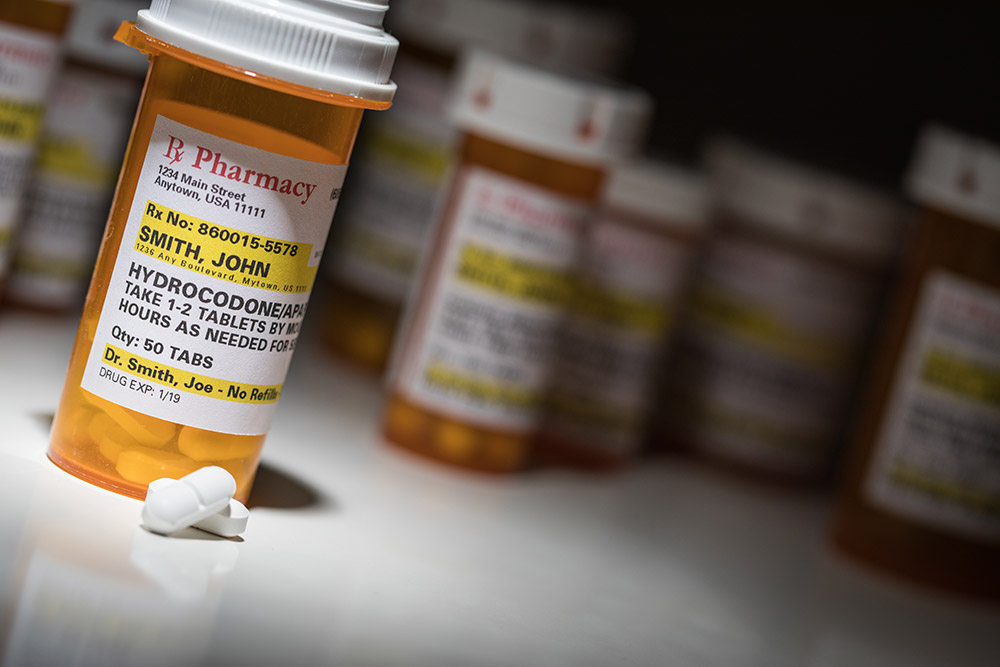
Opioids are analgesics (or painkillers) prescribed by doctors to treat pain. They work through having a depressant effect on the central nervous system. The NHS and private practices provide opioids in the treatment of acute pain, often linked to surgery or injury, and also for end-of-life care. These medications are especially useful in the treatment of terminal cancer and degenerative diseases, such as rheumatoid arthritis.
Opioids are semi-synthetic (man-made) opiates that bind to the opiate receptors in the brain. Opiates are derived from opium, a natural chemical found in the opium poppy. The terms “opiate” and “opioid” tend to be used interchangeably.
Opiates and opioids include:
- Codeine
- Fentanyl
- Heroin
- Hydrocodone
- Morphine
- Methadone
- Oxycodone
- Pethidine
Aside from heroin, which is an illegal street drug, all the opioids in this list can be prescribed by doctors.
While opiates are effective in short-term treatment, in the UK, the common consensus is that opioids should be avoided in the treatment of chronic or long-term pain. This is due to the high risk of opiate addiction and dependency.
What makes opioids so addictive?

Opioid addiction develops when you come to rely on the medication to feel “normal”. The original “high” is no longer present, and critically, withdrawal symptoms manifest as the opiate starts to leave the body. Withdrawal can be so distressing it causes you to keep returning to the substance even when you don’t want to (known as relapsing).
Opiates have a psychoactive effect on anybody who takes them. These substances directly impact receptors in your brain. In particular, the part of the brain which causes you to feel pain and pleasure. They also have a sedative effect. Opioids actually mimic endorphins, a naturally occurring brain chemical that relieves pain and causes a “natural” high.
The difference between endorphins and opioids is that the latter is far more powerful. Opiates create euphoria. For some people, especially those more susceptible to addiction, the brain’s reward system goes into overdrive. This is significant in compelling a person to return to the substance.
Opiate abuse occurs when you take your opioid prescription outside of recommended guidelines. This includes taking another person’s prescription, which is illegal.
Opiate addiction in the UK
Opiates are available legally and illegally in the UK. Legal use includes a prescription from a doctor, where you follow dose guidelines. If you have an opioid prescription but take more than is advised, this is a sign of opiate addiction. Illegal use includes taking opioids that were prescribed for someone else and taking illegal opiates, such as heroin.
It’s difficult to know the full gravity of opiate addiction in the UK. It was reported by The University of Manchester, however, that in England, between 1998-2016, opioid prescriptions more than doubled. It’s likely that many people on an opioid prescription might have developed opioid addictions without realising it. For many, it’s not until they try to stop the medication that difficulties present and dependency becomes apparent.
In relation to “high-risk opioid users”, the government estimates that there are 337,574 people aged fifteen to sixty-four addicted to heroin and fentanyl. This is the highest rate in the EU. It’s safe to assume that there are people who have been missed from these stats, who weren’t considered “high risk” but do have opioid addictions.
How opiates affect your health

Opioid addiction depresses the central nervous system. Immediate and long-term health effects include:
- Breathing problems
- Respiratory failure
- Constipation
- Nausea
- Confusion
- Drowsiness
- Reduced heart rate
- Physical changes in brain chemicals and structure
- Hormonal dysregulation
- Deterioration of mental health
- Deterioration or organs
- Reduced effectiveness of the immune system
- Increase in falls and fractures
- Risk of overdose
How to prevent opiate overdose
Overdose can be accidental. If you have an opioid prescription, it’s imperative to follow your doctor’s guidance regarding the dosage. Also, it’s critical not to mix opiates with other substances, especially other sedatives, such as alcohol, benzodiazepines or ketamine.
Physical signs of an opiate addiction
There are signs you can look out for if you’re concerned that you might have developed an opiate addiction. In relation to physical symptoms, it can feel very uncomfortable when the substance starts to leave your body. Physical dependency occurs when you find it impossible to function without the opioid.
Signs of opiate addiction include:
- Increasing the dosage to higher than your doctor’s advice.
- Mixing substances to feel an effect, which increases the risk of overdose.
- Participating in risky behaviours such as driving, operating heavy machinery and unprotected sex under the influence.
- Physical effects such as liver disease and damage to the brain, resulting in impaired cognitive functioning.
The most obvious physical signs of opioid addiction are experiencing withdrawal symptoms. It might take six hours to feel withdrawal from a short-acting opioid, whereas a longer-acting opioid might take thirty hours before you experience the symptoms.
Physical withdrawal symptoms include:
- High blood pressure
- Rapid heartbeat
- Flu-like symptoms
- Sickness and diarrhoea
- Pain and muscle spasms

Psychological signs you have an opioid addiction
The psychological signs of addiction might take longer to notice. Often, people find it easy to hide opioid abuse in the early stages, but as time goes on, the signs are clear. Despite this, it can be really difficult to accept, especially where you have full trust that a doctor has prescribed medication to help you.
Psychological symptoms are as follows:
- Thinking about and wanting opioid medication more often.
- Becoming secretive, withdrawn, and isolated.
- Having mood swings. Cravings can lead to aggression and rage, as well as low moods, depression, and anxiety.
- Losing interest in usual activities and hobbies.
- Neglecting responsibilities.
- Continuing to use opioids despite negative effects on your health, family, job or education.
How to tell if someone you love is addicted to opioids
There are signs you can look out for if you’re worried that someone you love is an opioid addict. In the earlier stages, you might notice your loved one starting to lose interest in usual activities. Perhaps they’re spending time with new people or becoming increasingly isolated. You might find paraphernalia (i.e. prescription bottles, blister packs, tin foil, plastic pen cases, and burnt spoons) around the home.
Sadly, many families experience the distressing effects of being manipulated, lied to, and stolen from. These behaviours can be especially challenging to live with. With the power of hindsight, you might realise how much your loved one’s behaviour has changed. It might feel as though they’re a different person. Mood swings are also very common as a person rides the ups and downs of cravings, withdrawal, and emotional dysregulation.
It’s important to remember that while you might see the signs, you’re loved one could be in denial of the addiction. This is difficult. At times like this, it’s important to try and maintain healthy communication so that your loved one will open up when they’re ready.
Signs of an opioid overdose
If your loved one displays signs of an overdose, including slow breathing, trouble staying away, pinpoint pupils, pale face, bluish lips and nails, clammy cold skin, confusion, disorientation, sudden mood swings, uncontrollable vomiting, low blood pressure, call emergency services.
Can you recover from opioid addiction?

Understandably, you’ll probably have many mixed emotions wondering whether you have an opiate addiction and, if so, what happens next. Although quitting opiates can be challenging, it is possible for you to recover from opioid addiction.
How to heal from opiate addiction
The best way to heal from opiate addiction is to stay as a resident at a rehab clinic. Our experienced team at UKAT can support you through opiate detox. This will lead you to the first step of recovery: removing the physical dependence. At opiate rehab, you’ll also develop the skills and techniques to regain control and create healthy new habits.
To find out more about detox and which of our clinics would suit your needs, contact our friendly team today.
Frequently asked questions
Keep an eye out for a change in performance at school, new friends, mood swings and a sudden lack of interest in hobbies. If behavioural changes are coupled with physical symptoms such as constricted pupils, changes in appetite and fatigue, your child may be suffering from opiate addiction, and it’s important to act quickly.