Eating disorders
Eating disorders are serious mental health conditions that can happen to anyone regardless of gender, age, and background. If left untreated, eating disorders can wreak havoc on a person’s body, mind, and life, and in some tragic circumstances, eating disorders can cause fatal consequences. Figures for the number of people suffering from different types of eating disorders vary hugely. Research suggests that there are 1.6 million Britons currently suffering from an eating disorder. But many sufferers do not seek help, so it is likely the actual number is even higher. If you think you or someone you love is struggling with an eating disorder, you may be feeling worried about their wellbeing, we understand your concern and we hope to assure you that eating disorders are treatable. So, let’s take a close look at the different types of eating disorders, their common symptoms, possible causes, and the best way to recover.

What are eating disorders?
Arguably, there is a greater awareness of eating disorders as mental health conditions now than ever before. However, stigmas around eating disorders still exist, one common misconception is: if you have anorexia, simply eat more and gain weight; If you binge eat- just eat less. It is likely anyone suffering from eating disorders will have heard these things countless times, often said by frustrated loved ones with good intentions, but invariably do more harm than good. Sadly, the reality for people with eating disorders isn’t so simple; for people suffering, issues around food and eating can dominate and disturb their waking lives in ways that they may feel powerless to control. Therefore, eating disorders are classified as behavioural addictions.
Types of eating disorders
There are many different types of eating disorders, and often, some disorders overlap. Let’s examine the most common ones:
Anorexia Nervosa (Anorexia)
Anorexia is characterised by the attempt to keep weight levels as low as possible by not eating. Sometimes, this is accompanied by purging or exercising in excess to burn calories. Anorexia is characterised by extreme body dissatisfaction, further fuelled by ingrained fear of gaining weight and a fixation with being thinner, no matter how much weight has been lost. Contrary to common misconceptions, the desire to be thin isn’t always motivated by unattainable beauty standards, it can also stem from a need to control, and often this impulse occurs in high-achievers or people who feel a compulsive pressure to be ‘perfect’- whether in school, work, or life in general.

Bulimia Nervosa (Bulimia)
Bulimia is an illness in which the person binge eats and then purges, most often through self-induced vomiting or taking laxatives or diuretics. Sometimes, the person may not regularly purge, but instead, exercise intensively in compensation for the binges. Binge eating in people with bulimia generally involves large amounts of food, often high in sugar and carbohydrates, that may be consumed rapidly and secretly until the person reaches extreme fullness. The binge may be planned or unplanned and is often triggered by stress, negative mood or extreme hunger resulting from intensive exercise between binges.
Binge Eating Disorder
Binge eating disorder is characterised by binge eating large amounts of food in short periods of time, on a regular basis, and without purging afterwards. People who binge eat might feel a lack of control over their eating, often eating rapidly, alone, and until they are uncomfortably full. They may also feel strong negative emotions regarding their eating, often feeling depressed, guilty, or disgusted with themselves after overeating.
Common signs and symptoms of eating disorders
If you think someone you love is struggling with an eating disorder, examine the table below to see if you recognise familiar habits which may indicate they have one of the above eating disorders.
| Anorexia | Bulimia | Binge Eating Disorder |
|---|---|---|
| Excessive weight loss | Eating a large quantity of food in a short amount of time | Eating large quantities of food when stressed |
| Obsessive body image | Feeling guilt or shame after eating | Eating when feeling lonely or bored |
| Refusal to eat meals with others | Frequently going to the bathroom after eating to vomit | Low self-esteem |
| A fixation on calories/obsessive counting | Excessive exercise to burn calories after eating | Fluctuation: weight loss or gain |
| Wearing boggy clothes to hide thinness | Colloused knuckles from vomiting | An impulse to eat when feeling sad or angry |
| Disrupted menstrual cycle – females will usually miss a period or periods may stop | Using laxatives to purge the body of food | Stomach cramps, constipation or acid reflux |
Common signs and symptoms of eating disorders
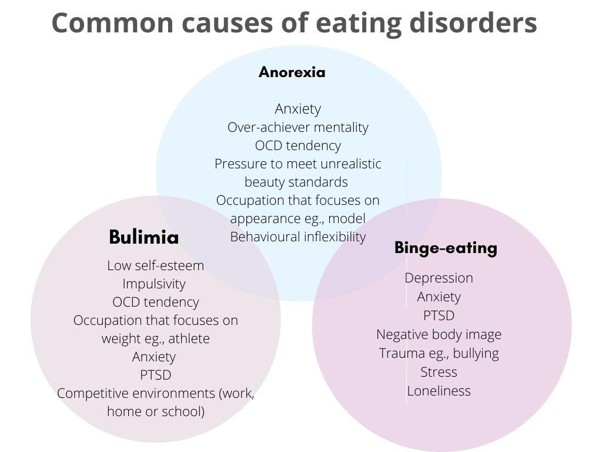
As you can see, various factors contribute to developing eating disorders, and each of the above conditions shares some potential causes. Most people struggling with eating disorders tend to have a co-occurring disorder as well. Anxiety, for instance, is a common factor in all eating disorders, and research has suggested that eating disorders, like other mental health issues, can be hereditary. If a sibling or a parent suffers from an eating disorder or co-occurring mental health issues, a family member is more likely to have similar struggles.
Environmental and cultural aspects can also give way to eating disorders; this can range from an inherent pressure to achieve perfection, to look a certain way for a job or sport, and pressure to meet society’s unattainable beauty standards. Another common denominator in eating disorders is low self-esteem and negative thought patterns surrounding body image. This may be further exacerbated by social media, as many young people associate their sense of self-worth with physical appearances and therefore try to emulate edited and unrealistic pictures of body shapes.
The health risks of eating disorders
The dangers of Anorexia
Of all the eating disorders, anorexia poses the most serious and immediate health concerns, both physical and psychological. According to the National Institute for Health and Care, the mortality rate of people with anorexia is 9.6%, which is about three times higher than any other psychiatric illness. Starvation affects every area of the body, and so physical health risks can be severe. Some of the most common health risks include:
- Osteoporosis
- Worn, painful teeth
- Severe dehydration
- Fatigue and weakness
- Absent periods
- Risk of heart failure
The dangers of Bulimia
As with Anorexia, the physical health risks posed by Bulimia can be incredibly varied. Yet where the dangers of Anorexia are largely linked to the impacts of starvation, the health problems associated with Bulimia are invariably rooted in the effects of the binge and purge cycle on the digestive system. This, in turn, can lead to electrolyte and chemical imbalances which can cause damage throughout the body, including to the heart and other major organs. Common health risks include:
- Tooth decay
- Oesophageal tears
- Chronic irregular bowel movements
- Pancreatitis
- Stomach rupture
- Type 2 Diabetes

The dangers of Binge-eating disorder
The physical complications caused by binge eating can be twofold. First are the more immediate effects on the digestive tract, which in turn can lead to problems throughout the body. If continued over time, this can lead to obesity and all of the health risks associated with the condition. Over two-thirds of people with binge eating disorders are overweight or obese. Common health risks include:
- Obesity
- Gallbladder Disease
- Sleep apnea
- Stomach rupture
- Type 2 diabetes
- high cholesterol
The Psychological risks of all eating disorders
While the physical effects of bulimia and anorexia are quite different, the mental health problems associated with both illnesses share much in common. For both, there is a crossover between underlying mental health traits, and psychological disorders arising from the chemical imbalances caused by difficult eating habits:
- Depression
- Obsessive compulsive disorder
- Anxiety
- Poor concentration
- Loneliness
- Isolation
In terms of binge-eating disorders often, the psychological difficulties come first, a ‘comfort’ mechanism to boost the mood. However, this can lead to feelings of guilt and low self-esteem, which can, in turn, lead to further bingeing, beginning a ferocious cycle that can be hard to break.

Eating disorder treatment: the best way to recover
UKAT understands that the above outcomes for each eating disorder can seem scary, but we want to assure you that life-threatening outcomes are worst-case scenarios, and many people receive treatment for eating disorders before things deteriorate for the worse. Therefore, it’s imperative to seek out rehabilitation treatment as soon as possible. So, take comfort in knowing that reading this page alone is an excellent first step towards recovery.
Eating disorders treatment options
In the medical community, eating disorders are often referred to as being psycho-physical, meaning treatment must look at the mind and body together. Whether we are talking about anorexia, bulimia or binge eating disorder – all must be approached holistically under the guidance of expert therapists and medical professionals.
Treatment programmes will be tailored closely to the specifics of each patient, considering not only the type of eating disorder they suffer from but also the possible co-occurring disorders and influences which make up their personal situation. This should be clear from the outset, so the first step in most treatment programmes will be for a doctor to carry out a physical assessment to ascertain any immediate danger the patient may be in and how the body can be restored to good health. This will lay the foundations for a thorough dietary programme, which will be accompanied by dietary counselling throughout treatment.
If any of the information on this page has resonated with you, know that you are not alone, and we are here to support you. Banbury Lodge, UKAT’s rehab centre based in Oxfordshire, specialises in treating eating disorders and offers a variety of programmes tailored to help you reach a healthy recovery. A life free from the clutches of addiction is possible, and with the proper support, you can regain control of your life and move towards a healthier future.

Therapies for eating disorders
Following this, a personal assessment is conducted by a therapist. This will allow the remainder of therapy to be tailored to the patient’s needs. A trained psychologist will work with patients to understand the underlying reasons behind their eating disorders. Plus, several types of therapy will also be offered including family counselling, psychotherapy, Cognitive behavioural therapy, and group therapy. All have proven to be immensely effective in eating disorder recovery.
We see people recover from the crippling effects of eating disorders often, so we want you to know there is hope; if you are suffering from an eating disorder or care about someone who is, know that it is treatable, and people do reclaim their physical and mental health before going on to live a good quality of life.