Written by:

Medically Reviewed by:
Last Updated:
May 12th, 2026
Alcohol addiction
Alcohol addiction, also known as alcohol use disorder, is when drinking shifts from something occasional or social into something that begins to take control. It can look different for each person: some may drink daily, others only in bursts but the common thread is the impact alcohol has on the person’s life and the people around them. For many, this change happens gradually, making it difficult to recognise until alcohol is firmly in the driver’s seat.
What is Alcohol?
To understand alcohol addiction, it is first important to understand what exactly alcohol is and how it effects the human mind and body;
What is an alcohol addiction?
The Diagnostic and Statistical Manual of Mental Disorders (DSM-5) outlines alcohol use disorder using a set of criteria. Below, we take a look at just a few of these criteria:
- Drinking more alcohol or for longer than originally intended.
- Trying to cut down or stop drinking but not managing to do so.
- Spending large amounts of time getting alcohol, drinking it or recovering afterwards.
- Strong cravings or urges to drink.
- Drinking that disrupts responsibilities at work, home or school.
- Continuing to drink even when it causes problems in relationships.
- Experiencing withdrawal symptoms when not drinking or drinking to avoid them.
Clinicians use these criteria to assess the severity of alcohol addiction: meeting two to three is considered mild, four to five is moderate, and six or more is severe. But beyond the numbers, the real measure is whether alcohol feels like it is controlling you more than you are controlling it.
What does an alcohol addiction look like?
In places where alcohol is not only legal but almost encouraged at every social gathering, it can be hard to know where “normal drinking” ends and something more troubling begins. Society tends to picture alcoholism in extremes: the person on the street with a bottle hidden in a paper bag, dishevelled, ill and struggling. That image is real but it only represents one part of alcoholism, the later stage.
What gets lost in that stereotype is everyone who doesn’t fit it. The person who makes it through the workday with a smile, only to drink in secret at home. The friend who stays sober Monday to Friday but goes on weekend benders that leave their body reeling. Even those who appear “in control” may already be caught in the web of alcohol addiction.
The truth is, alcoholism is a process that unfolds in stages, and that’s what the Jellinek Curve was designed to show. Created in the 1940s and still used today, it helps us see how alcohol addiction develops gradually rather than suddenly appearing in the way most people imagine.
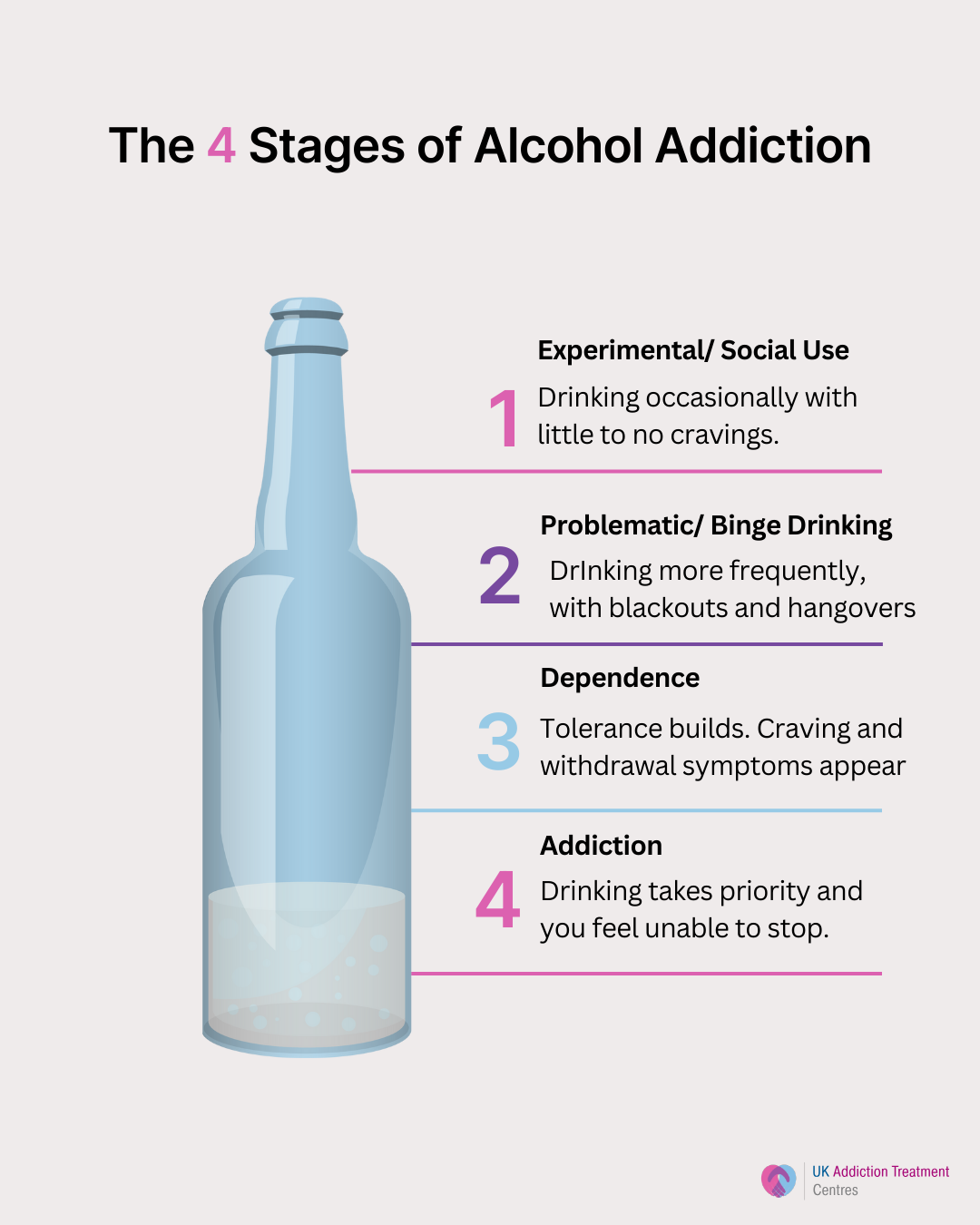
- Early stage: Drinking feels positive, lowers stress and acts as a reward. Habits start to form quietly in the background.
- Middle stage: Alcohol becomes something to rely on. People may drink secretly, make excuses or cancel plans that don’t involve alcohol.
- Late stage: Health, relationships and finances suffer and drinking often happens to avoid withdrawal rather than for pleasure. This is the version of alcoholism most people recognise.
- Recovery stage: The curve also shows recovery is possible, with people able to regain health, stability and connection when the right support is in place.
The importance of this model lies in what it reveals: alcohol addiction doesn’t only exist in its most visible, late-stage form. It can be present long before anyone else notices, hidden behind appearances that seem perfectly intact.
What makes alcohol addiction so dangerous?
We all know alcohol addiction is bad; that part doesn’t need explaining. But if you haven’t lived through it yourself or seen someone close to you go through it, it’s easy to overlook just how deep the damage runs. The truth is, alcohol doesn’t just affect one area of life. It pulls at health, relationships, finances, and even the basic act of stopping drinking can turn into a risk.
At UKAT we can help you discover to best options for a clear path forward.
Alcohol addiction in the UK
The UK has always had a close relationship with alcohol. Parties, weddings, football nights, even a quiet Saturday evening, more often than not, a drink is part of the picture. Spotting the alcohol is easy. Spotting the person quietly struggling with it is far harder. If we think back to the Jellinek Curve, we know just how well those struggles can be hidden. What isn’t hidden is the toll alcohol addiction is taking on lives and communities across the country.
Below are some of the most shocking alcohol stats to come out of the UK in recent years:
While some of the figures above may reflect isolated alcohol-fuelled incidents rather than outright addiction being the cause, research suggests there are around 608,416 people in the UK who are alcohol dependent.
The reality is that this figure falls short of the truth, as many people never seek alcohol addiction treatment and so are not captured in the data, while others may not even recognise their drinking as an addiction. With this in mind, the connection between those wider statistics and alcoholism feels much closer than it first appears.
How can I spot alcohol addiction in myself or others?
After looking at the scale of alcohol addiction across the UK, it’s only natural to start thinking closer to home, about your own drinking or that of someone you care about. Spotting the signs early can make all the difference but because alcohol is so common in everyday life, these signs are not always obvious. Below, we’ve broken them into three areas to help bring some clarity.
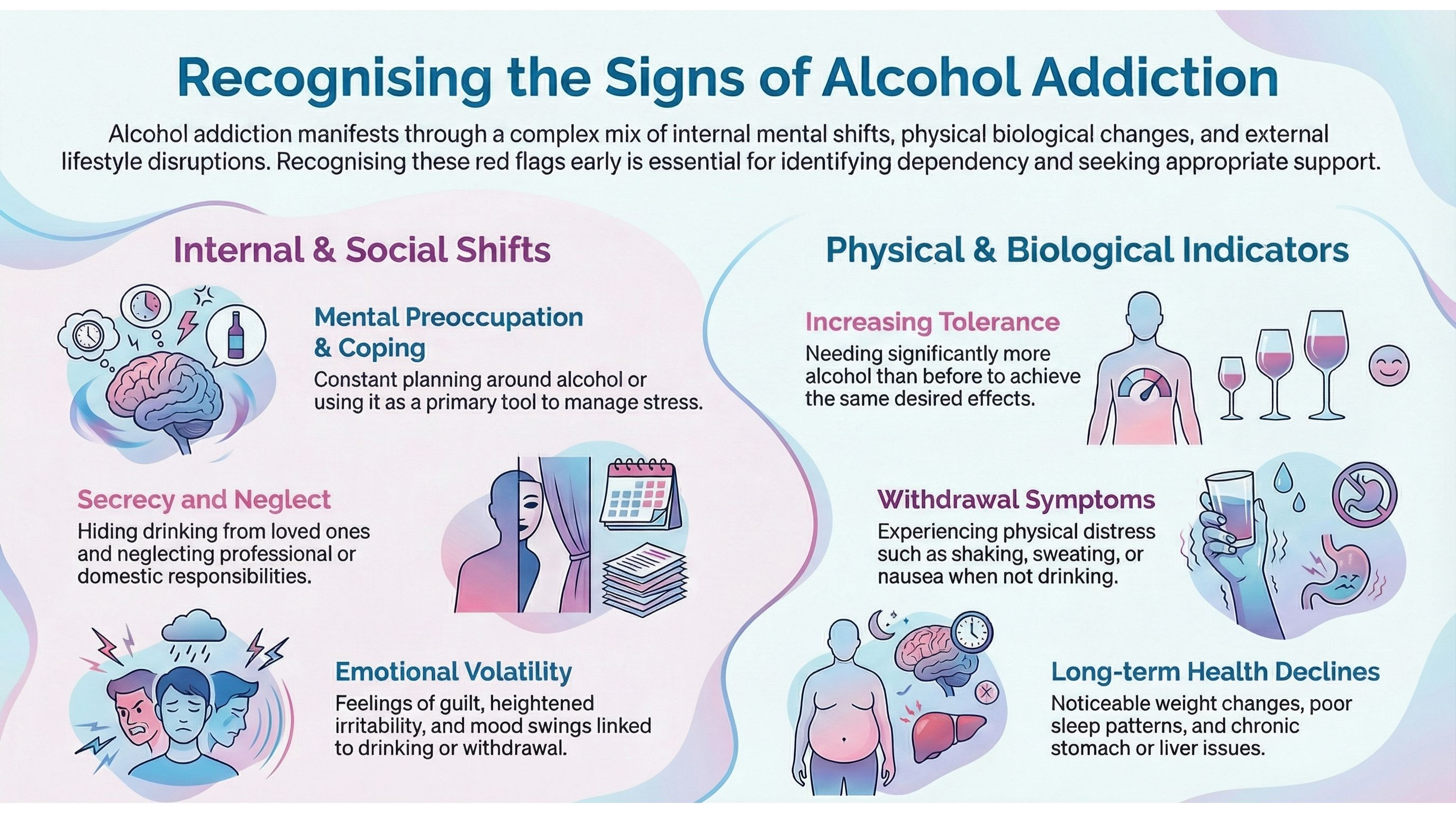
- Constant preoccupation with drinking, such as planning the next drink or worrying about when alcohol will be available.
- Using alcohol as a way to cope with stress, anxiety or low mood.
- Feeling guilt or shame about drinking habits but finding it difficult to cut down.
- Heightened irritability, mood swings or depression linked to drinking or withdrawal.
- Needing more alcohol to feel the same effects (increasing tolerance).
- Regular hangovers or withdrawal symptoms such as shaking, sweating or nausea.
- Noticeable weight changes, poor sleep patterns or ongoing health complaints.
- Developing alcohol-related illnesses, such as stomach issues or liver problems.
- Hiding drinking from family, friends or colleagues.
- Neglecting responsibilities at work, home or school because of alcohol use.
- Social withdrawal from activities where drinking isn’t involved.
- Risky behaviours, such as drunk driving or unsafe sex, when under the influence.
If you’ve noticed some of these signs in yourself or someone close to you, it could mean help is needed. A good way to do that is by asking some direct, honest questions. The next section offers a short self-questionnaire designed to help you reflect on whether alcohol has started to play too big a role in your life.
Do I have an issue with alcohol?
If any of the topics we’ve covered today have shone a light on your drinking habits or those of people you love, it’s always worth checking in with yourself. Addiction of any kind has a way of hiding in everyday life, which is why a moment of honest reflection can sometimes be the turning point you never expected.
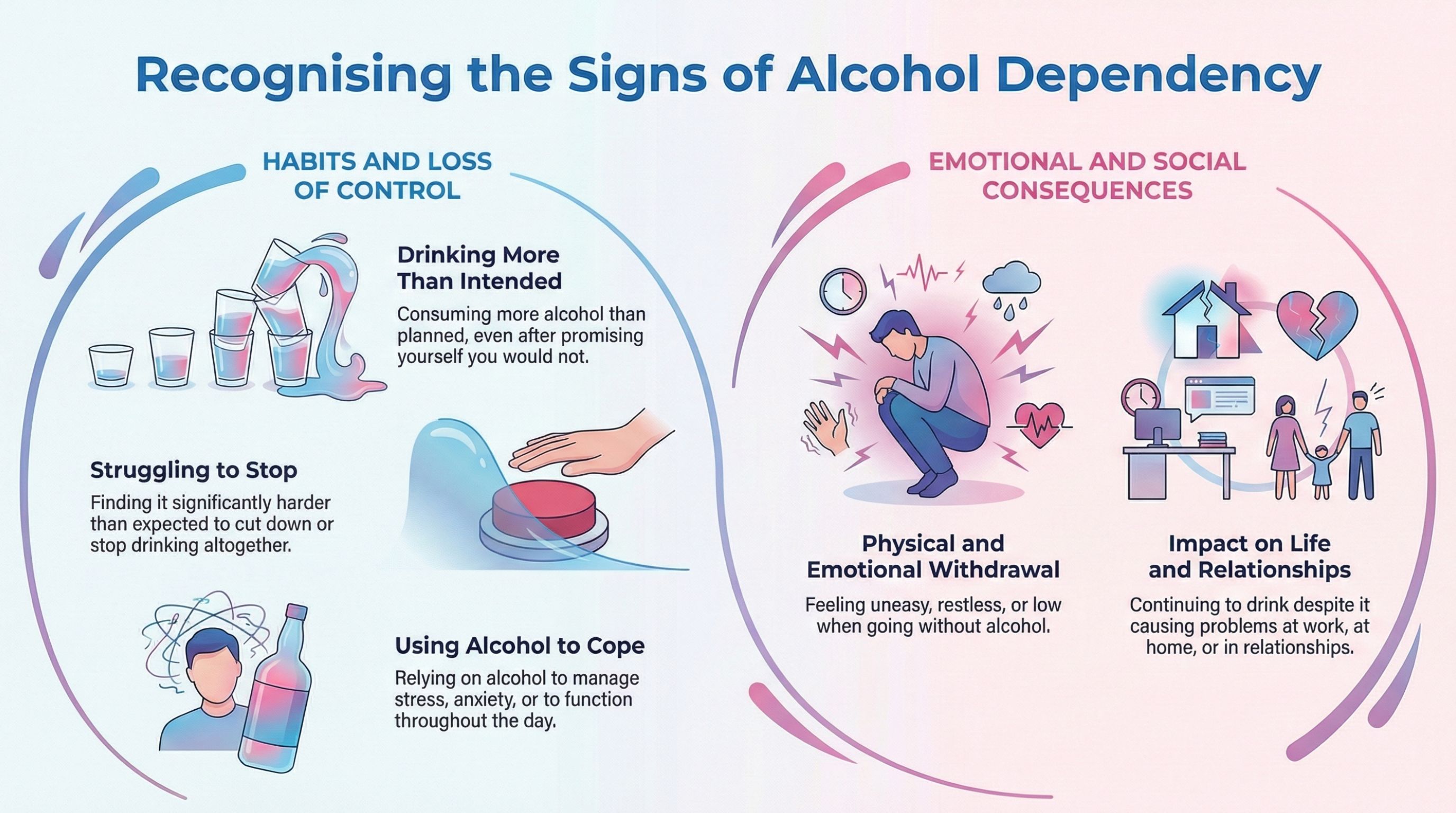
- Do you often end up drinking more than you first intended, even when you promised yourself you wouldn’t?
- Have you tried to cut down or stop altogether but found it harder than expected?
- Do you feel uneasy, restless or low when you go without alcohol?
- Has drinking caused problems at work, home or in your relationships, yet you’ve carried in anyway?
- Do you find yourself needing alcohol to cope with stress, anxiety or just to get through the day?
If some of these questions feel uncomfortably familiar, take it as an important signal rather than something to ignore. The next section will guide you toward the types of support available and how reaching out for help can open the door to change.
Where can I find help for alcohol addiction?
If you’ve recognised signs of alcohol addiction in yourself or someone close to you, it’s important to know that help is always available. At UKAT, we provide treatment options that include safe, medically supported alcohol detox and structured rehab programmes, giving people the chance to step away from alcohol and begin building a healthier future. Our centres offer supportive environments where recovery can start, guided by professionals who understand both the challenges and the hope that come with change.
Taking that first step may feel overwhelming but it can also be the moment where life begins to move in a new direction. If you’re ready to explore support for yourself or for a loved one, reach out to UKAT today and discover how we can help.
Reach out today to find out how UKAT can help you get past your alcohol dependence.
Frequently asked questions
Alcohol is often used as a coping mechanism to deal with trauma. An addiction develops when you are unable to cope with the symptoms of those conditions without alcohol.
Assess your alcohol dependence with the CAGE questionnaire for alcohol addiction
(Click here to see works cited)
- American Psychiatric Association, DSM-5 Task Force. (2013). Diagnostic and statistical manual of mental disorders: DSM-5™ (5th ed.). American Psychiatric Publishing, Inc.. https://doi.org/10.1176/appi.books.9780890425596
- JELLINEK, E. M. “Phases in the Drinking History of Alcoholics.” Quarterly Journal of Studies on Alcohol, vol. 7, June 1946, pp. 1–88, pubmed.ncbi.nlm.nih.gov/20989144/
- NHS. “Risks – Alcohol Misuse.” NHS, 4 Oct. 2022, www.nhs.uk/conditions/alcohol-misuse/risks/
- Newman, Richard K., et al. “Alcohol Withdrawal Syndrome.” Nih.gov, StatPearls Publishing, 2024, www.ncbi.nlm.nih.gov/books/NBK441882/
- Alcohol-Specific Deaths in the UK: Registered in 2023. backup.ons.gov.uk/wp-content/uploads/sites/3/2025/02/Alcohol-specific-deaths-in-the-UK-registered-in-2023.pdf
- Office for Health Improvement & Disparities. “Alcohol Profile: Short Statistical Commentary, February 2025.” GOV.UK, 4 Feb. 2025, www.gov.uk/government/statistics/alcohol-profile-february-2025-update/alcohol-profile-short-statistical-commentary-february-2025
- Department for Transport. “Reported Road Casualties in Great Britain, Involving Illegal Alcohol Levels: 2023.” GOV.UK, 30 July 2025, www.gov.uk/government/statistics/reported-road-casualties-in-great-britain-involving-illegal-alcohol-levels-2023
- Balogun, Bukky and Joshua O’Loughlin. “Alcohol and Cancer.” House of Commons Library, 8 July 2025, commonslibrary.parliament.uk/research-briefings/cdp-2025-0157/
- Office. “Estimates of Alcohol Dependent Adults in England: Summary.” GOV.UK, 14 Mar. 2024, www.gov.uk/government/publications/alcohol-dependence-prevalence-in-england/estimates-of-alcohol-dependent-adults-in-england-summary